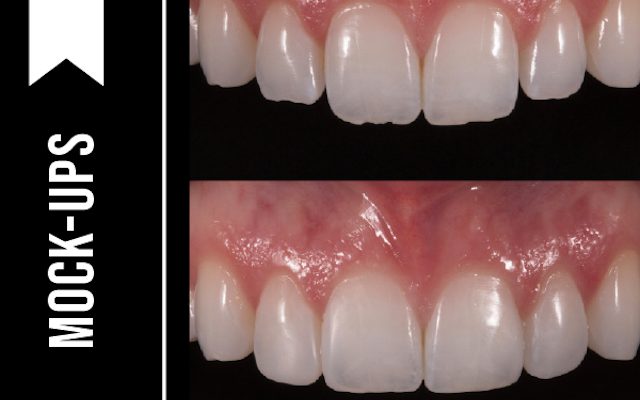
Implants are replacements for teeth—they are not teeth. This might sound obvious, but it’s a simple reality implant surgeons must remember, as there are key differences between natural teeth and implants that must be observed.
Understanding the differences
The periodontium is composed of bone, periodontal ligament and connective tissue. The fibers around the tooth insert horizontally, tangentially and circumferentially, wrapping the tooth securely and supporting it against trauma.
This simple yet complex arrangement is very strong, and is nourished by an abundant blood supply coming from the periodontal ligament and periosteum. This is why teeth are resistant to bacterial assaults and, in most cases, why periodontal disease is slow-moving and chronic.
Implants, on the other hand, have a hemi-desmosomal attachment. The fiber arrangement around implants is more commonly parallel. That means the thinner the tissues, the more fragile the attachment. Because there is no periodontal ligament to offer blood supply, blood supply is limited to the periosteum.
Fiber arrangement and blood supply are factors that lead to vulnerable osseous tissue and could result in earlier bone marrow penetration when infection sets in. It is believed this is why we see aggressive, cupping-type bone loss around dental implants in peri-implantitis.
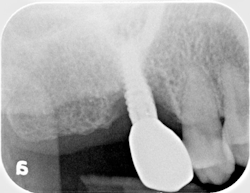
Assessing the soft tissue before implant placement
One common pitfall for implant surgeons is only answering the most commonly asked question: “Does this patient have enough bone for an implant?”
While it is true no bone equals no implants, it is also true that if there isn’t healthy tissue, there is a greater chance there will not be long lasting healthy implants. Patients who come to us for implants don’t want a short-term solution. They want healthy implants that offer long-term success. As implant therapists, we must identify what type of tissue will be present around our implants and prosthesis when treatment is complete, and intervene when these tissues are not optimal for long-term success.
It’s vital to take the time to measure attached keratinized tissue before planning surgery, and to educate patients about the importance of maintaining healthy attached keratinized tissue around their implants. Dentists should explain the techniques available for both full site bone and soft tissue development.
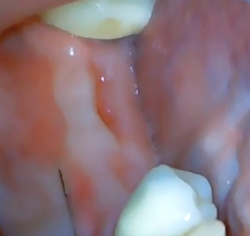
Protecting existing soft tissue, and methods for creating protective soft tissues for implant health
When planning implant surgery, it’s important to think carefully about incision design. Some implant surgeons use punch techniques when placing dental implants because they’re uneasy about reflecting a full flap. This common error leads to thin zones of attached keratinized tissue being removed, which sets patients up for peri-implantitis down the road. Using punch or laser uncovering is another potential pitfall when preserving attached tissue.
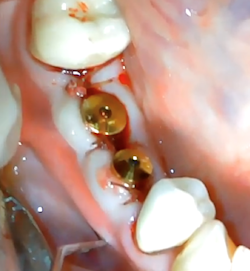
Don’t forget the basics
Spend extra time discussing proper maintenance with patients who have natural dentition. We must teach our implant patients proper hygiene techniques and provide them with the right tools to use at home.
Cleaning around these complex restorations is not intuitive. To set them up for success, we must spend time teaching patients how to properly care for their implants. There are specific, well-designed implant hygiene tools on the market, but they are not always readily available at their local pharmacy or store. The responsibility falls on us to educate patients on how to use these tools. Proper maintenance will help keep their soft tissues healthy so they can continue to be the first line of bacterial infiltration defense.
Parting thoughts
Dentistry has an obligation to advance the science of dental implants in armentarium, diagnosis and surgical technique. The future is bright for our patients as long as we, as the therapists, respect the biologic basics of the system we’re treating.
 By:
By: